Prepared by Mike Yarmo, VP, SIMAC Canada Inc.
Special thanks to Dr. Randy Silverman, Psychologist, who consulted on this article.
INTRODUCTION
An automobile accident can potentially be a traumatic event in a person’s life. Transport Canada’s National Collison Database reports that there were 160,000 automobile accidents last year, with nearly 50% resulting in some form of personal injury, which has created a major burden for society to bear. Injuries can manifest both physically and mentally, leaving victims with a potentially long road to recovery.
For auto accidents in Ontario, there is a well-defined recovery plan, with injured individuals entitled to different levels of benefit spending, depending on the severity of the injury, which range from minor injuries managed under the Minor Injury Guideline (“MIG”) to catastrophic claims. In the event that the victim has suffered a minor injury, defined as one or more of a sprain, strain, whiplash, contusion, abrasion, laceration or any clinically associated sequelae, the MIG includes a $3,500 medical and rehabilitation benefits budget.
Depending on the treatment plan, should the injuries be deemed minor, the $3,500 could be quickly exhausted. In the event of a compensation claims dispute, a claimant may resolve the issue before the Licence Appeal Tribunal (“LAT”), with arguments designed to establish that their injuries should be considered “outside the MIG”. In a recent sample of LAT decisions, psychological impairments were cited in nearly 50% of cases in which it was argued that their injuries were more severe, which would propel the budget from $3500.00 under the MIG up to $65,000 for non-catastrophic injuries.
Understanding the risk, upon receiving an unfavourable LAT decision, every party responsible for the resolution of a claims dispute should consider the question as to whether “the risk of suffering from a psychological impairment can be predicted before an automobile accident?”, which would mitigate the risk of a claims compensation dispute.
DEEPER DIVE INTO PSYCHOLOGICAL IMPAIRMENTS
Psychological impairments are often precipitated by a traumatic event, like an automobile accident, and can significantly impact a person’s interpersonal/familial relationships, work productivity, and overall quality of life. According to the Canadian Mental Health Association, psychological impairments can be categorized into three main categories…
| Psychological Impairment Categories | Additional Details |
|---|---|
| Post-Traumatic Stress Disorder (“PTSD”) | Only shows up weeks after an accident |
| Persistent Anxiety (“PA”) | Present for weeks to months after the accident |
| Major Depressive Disorder (“MDD”) | Depression unresolved with 2+ anti-depressives |
Courts have recognized that mental injuries should be compensated at the same level as physical injuries, with the Supreme Court of Canada ruling in the case of Saadati v. Moorhead, 2017 SCC 28, [2017] 1 S.C.R. 543 a the plaintiff suffered psychological damages after his tractor truck was hit by the defendant based on negligent driving. In this particular case, testimony was heard from lay witnesses, including family and friends, without expert evidence establishing an identifiable medical diagnosis1. The Supreme Court of Canada overturned a ruling by the BC Court of Appeals, restoring the awarded damages, with its ruling based on symptoms and effects rather than diagnosis.
With the high court of the land’s 2017 ruling, in the event that funding under the MIG is insufficient to address a psychological impairment, accident victim representatives have case precedence and clearer guidance on how to present their clients’ dispute, which represents a new risk factor for the P&C Insurance Industry, which should strongly consider taking decisive action for effectively managing potential additional claims payments.
The hypothesis this paper will start to address relates to whether “the risk of an accident victim suffering from a psychological impairment can be predicted before the accident happens”
RESULTS OF A PREDICTIVE STUDY
A 2020 European study published in the U.S.-based National Library of Medicine (“NLM”) concluded that there are predictors of the likelihood of an auto accident victim suffering from PTSD, PA or MDD, based on factors related to the persons health, lifestyle, and characteristics of the accident.
The NLM is operated by the United States federal government and is the world’s largest and most trusted source of health information that is utilized by health professionals, medical libraries, and research students. The study references over 40 different peer-reviewed studies2, and represents a strong starting point for exploring our hypothesis.
Diagram 1
| Category | Impairment Rate |
|---|---|
| PTSD | 32.3% |
| PA | 5.8% |
| MDD | 17.4% |
A sample of accident victims, independent of the seriousness of their injuries, was tested one-month post-accident, using a self-reported assessment of PTSD, PA and MDD. As shown in diagram 1, PTSD rates were significant in study participants, which is highly expected and consistent with widely available reports that auto accidents are a leading cause of PTSD3. Other studies have also shown PTSD rates as high as 45% in post-accident victims4.
MDD was also high, with nearly 1 in 5 respondents meeting its medical definition, while levels of PA were barely recorded above the base line and were not considered a major post-accident condition.
With the understanding that PTSD is recorded in a third to nearly half of all accident victims, a meta-analysis was conducted to determine whether there is a correlation to pre-existing conditions, as reflected by lifestyle, socio-economic, or health related factors, which can be used to predict individuals who are most at risk for being impaired by PTSD following their involvement in a motor vehicle accident.
Please note, the study excluded any victims…
- under 18 years old.
- suffering from major cognitive impairment due to an accident.
To assess the severity of the psychological impairment, all questionnaires utilized the Abbreviated Injury Scale (“AIS”) methodology, with a final score calculated with the New Injury Severity Scale (“NISS”). This scale system is an accepted method for testing trauma levels. It also provides clinicians with a quantitative score for ascertaining correlation levels. Questions for testing PTSD symptoms adhered to the DSM-IV.
Summary of pre-automobile accident sociodemographic and health status characteristics of study participants…
| Gender | Male – 55% | Female – 45% |
| Age | <41 – 50% | >=41 -50% |
| Residence | Urban – 42% | Rural – 58% |
| Education | University – 15% | No Univ – 85% |
| Employment | Employed – 58% | UE/Retired – 42% |
| Martial Status | Single – 38% | Coupled – 62% |
| Economic Status | Above Avg – 21% | Avg to Below – 79% |
| NO | YES | |
| Smoking | 63% | 37% |
| Alcohol | 49% | 51% |
| Religious | 10% | 90% |
| Medication Use | 49% | 51% |
| Prior Car Accidents | 59% | 41% |
| Previous Trauma | 47% | 53% |
| Previous PTSD | 97% | 3% |
| Pre-Chronic Illness | 58% | 42% |
| Pre-Psych. Illness | 89% | 11% |
| Previous Perm. Pain | 91% | 9% |
The predictive characteristics are organized into four major cohort groups…
- sociodemographic
- pre-accident health status
- severity of injury in the accident
- characteristics of the accident itself
The 4 cohorts have an accompanying heatmap (see below) that uses a colour-coded ranking system of green, yellow or red, with green representing a strong predictor of psychological impairment (i.e., based on what is known before or on the day of the auto accident), and yellow or red representing a poor(er) prediction attribute of psychological impairment.
The organization of the colour-coded ranking system is based on p-values scores (or probability that the observed difference between our test group and another group is random chance). Our null hypothesis is that there is no relationship between the characteristics and its ability to predict PTSD. However, the lower the p-value, the more significant the relationship is, rather than the findings being a result of random chance. Using this system, only the green attributes have sufficiently high correlations for predicting psychological impairment risk.
For example, the study found that level of economic status is a good predictor of whether the accident victim is at higher risk of suffering from MDD or PTSD. As stated before, 20%-50% of auto accident victims claimed to suffer from either MDD or PTSD. These types of reliable predictions would therefore promote more informed post-accident decisions from all stakeholders.
Focusing only on PTSD, there are only a few statistically significant pre-accident characteristics that are accurate predictors of psychological impairment, which include gender, economic status, and prior psychiatric illness, with the factors of the accident itself being a much stronger predictor of the risk of psychological impairment.
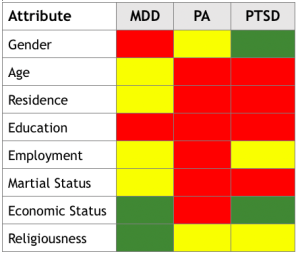
SOCIODEMOGRAPHIC FACTORS
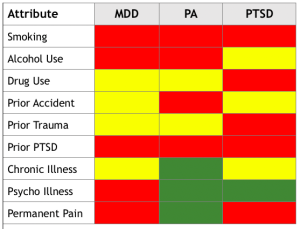
PRE-ACCIDENT HEALTH FACTORS
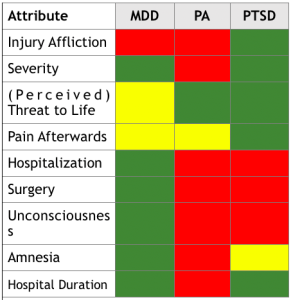
SEVERITY OF INJURY IN ACCIDENT
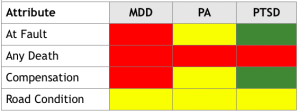
ACCIDENT CHARACTERISTICS
Accident victims with pre-accident characteristics that are strong predictors of psychological impairment represent 10% of the Canadian population and could be as high as 16.5% of the population, depending on the province. In Ontario, there were 74,172 auto collisions in 2022, with the number of high-risk exposed individuals between 7,500-12,500 (including witnesses and passengers). To the extent that the Ontario License Appeal Tribunal settles or hears 13,000 cases per year5, including physical and mental health cases, there is a significant number of people with high-risk characteristics who will likely suffer from some form of psychological impairment as a result of an automobile related incident, which could represent a significant differentiator for the first mover who incorporates this information in the P&C insurance space.
1. https://canliiconnects.org/en/summaries/45774
2. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7074414/
3. https://www.mayoclinic.org/diseases-conditions/post-traumatic-stress-disorder/symptoms-causes/syc-20355967#:~:text=The%20most%20common%20events%20leading,Sexual%20violence
4. https://www.injuryjournal.com/article/S0020-1383(13)00318-5/fulltext
5. https://tribunalwatch.ca/wp-content/uploads/2022/02/two-survey-licence-appeal-tribunal-report-final-2022-02-08.pdf

